Pneumonia
Pneumonia or pneumonia is a disease of the respiratory system that consists of infectious inflammation of the alveolar spaces of the lungs.
Pneumonia is usually an acute infection of the lung parenchyma associated with a new infiltrate on chest radiography. Pneumonia can affect an entire lung lobe (lobar pneumonia), a lobe segment, the alveoli close to the bronchi (bronchopneumonia), or interstitial tissue (interstitial pneumonia). Pneumonia causes the tissue that makes up the lungs to become inflamed, swollen, and painful. Many patients with pneumonia can be treated on an outpatient basis without requiring hospital admission.
Community-acquired pneumonia (CAP) or extrahospital pneumonia is that acquired outside hospitals, while nosocomial pneumonia (NN) or intrahospital pneumonia (NIH) is acquired during the hospital stay (after 48 hours after hospital admission). After 48 hours, the criteria for a new infiltrate is added to the chest X-ray. Signs of infection can be assessed by an increase in C-reactive protein (CRP), fever (>37.8 °C) or leukocytosis with a left shift (increased neutrophils).
Pneumonia can be a serious disease if not detected early, and can be fatal, especially among the elderly and the immunocompromised. AIDS patients in particular frequently contract pneumonia from Pneumocystis. People with cystic fibrosis are at high risk of pneumonia because fluid continually accumulates in their lungs.
It can be contagious, since the microorganisms that cause this disease spread rapidly in the air, and can be spread through sneezing, coughing, and mucus; A patient who has suffered from pneumonia can be left with sequelae of this in their body for a long time, this makes it potentially contagious and the people most likely to contract it are those who are in the process of flu or asthma, among other diseases of the system. respiratory. Cigarette smoking can also multiply the risk.
Treatment depends on the underlying cause. Pneumonia thought to be due to bacteria is treated with antibiotics. If the pneumonia is severe, it may require hospitalization. Oxygen therapy (hypoxemia) may be used if oxygen levels are low.
Pathophysiology
Cases of infectious pneumonia often present with a cough that produces brown or green sputum (phlegm) and a high fever that may be accompanied by feverish chills. Dyspnea (respiratory distress) is the most specific and sensitive early sign. Pleuritic chest pain is also common, (sharp or stabbing pain that comes on or worsens with coughing and deep breathing). People with pneumonia may cough up blood (hemoptysis), have headaches, or have clammy, sweaty skin. Other possible symptoms are lack of appetite, tiredness, cyanosis, nausea, vomiting, and joint or muscle pain. Less common forms of pneumonia can cause other symptoms, for example pneumonia caused by Legionella, which can cause abdominal pain and diarrhoea, while pneumonia caused by tuberculosis or Pneumocystis can only cause weight loss and night sweats. In older people, the manifestation of pneumonia may not be typical. They may develop new or more severe confusion, or experience imbalances, causing falls. Children with pneumonia may have many of the above symptoms, but in many cases they are simply sleepy or lose their appetite.
Symptoms of pneumonia require immediate medical evaluation. Physical examination by a healthcare worker may reveal fever or sometimes low body temperature, rapid breathing rate (tachypnea), low blood pressure (hypotension), elevated heart rate (tachycardia), or low oxygen saturation. (SatO2), which is the amount of oxygen in the hemoglobin well revealed by pulse oximetry or by arterial blood gases (GASA). Patients who have difficulty breathing (dyspnea), are confused, or have cyanosis (blue skin) and need immediate attention.
Physical examination of the lungs may be normal but often has decreased expansion (amplexion) of the chest on the affected side, bronchial breathing on stethoscope (harper sounds from the larger airways, transmitted through of the inflamed and consolidated lung) and perceptible rales in the affected area during inspiration. Percussion may be muffled (dull) over the affected lung, but with increased rather than decreased resonance (distinguishing it from a pleural reservoir). Although these signs are relevant, they are insufficient to diagnose or rule out pneumonia; in fact, studies have shown that two doctors can come to different conclusions about the same patient.
Viruses
Viruses need to invade cells to reproduce. Viruses normally reach the lung through the air, being inhaled through the mouth or nose, or by eating food. Once in the lung, the viruses invade the lining cells of the airways and alveoli. This invasion often leads to cell death, either directly or via apoptosis. When the immune system responds to the viral infection it causes further lung damage. Leukocytes, mainly lymphocytes, activate a variety of chemical inflammatory mediators such as cytokines, which increase the permeability of the bronchial alveolar wall, allowing the passage of fluids. The combination of cell destruction and the passage of fluids into the alveolus worsens gas exchange.[citation needed]
In addition to lung damage, many viruses infect other organs and can interfere with multiple functions. Viral infection can also make the host more susceptible to bacterial infection.
Viral pneumonias are mainly caused by influenza virus, respiratory syncytial virus, adenovirus. The herpes virus is a rare cause of pneumonia except in newborns. Cytomegalovirus can cause pneumonia in the immunocompromised.
The SARS-CoV-2 virus, which causes the COVID-19 pandemic, presents pneumonia in its severe cases. It was precisely the large number of cases of pneumonia of unknown origin reported in the Chinese province of Wuhan in December 2019 which caused the disease to be detected.
Classification
Pneumonia can be classified into:
- Depending on the causal agent:
- pneumococcal
- pneumonia staphoccal
- Pneumonia for Klebsiella
- Pneumonia for Legionella
- By anatomopathological involvement:
- Pneumonia alveolar or lobar: it affects multiple alveolos, which are filled with exudate and can even compromise a complete lobe; however, bronchioles are quite respected, which is why the radiological phenomenon known as Air drilling. This is the typical presentation of pneumococcal pneumonia.
- Multifocal pneumonia or bronconeumony: affects alveolos and adjacent bronchioles; the involvement is usually multiple segmentary, but it is rare that it affects a complete lobe; due to the involvement of bronchioles, the sign of the air bronchogram is not appreciated. In this way, the pneumonia of negative Gram and staphylococcus aureus.
- Interstitial pneumonia: as its name says it affects the area of the intersection, respecting the bronchial and alveolar light. It is usually the form of manifestation of viruses and other atypical or germs Pneumocystis jirovecii, although they may sometimes produce common bacteria.
- Necrotizing pneumonia and pulmonary abscess: some germs may produce necrosis in the pulmonary parenchyma, which radiologically appear as hyperlucent zones in the breast of a condensed area; depending on the fact that there is a single large cavity (up to 2 cm) or multiple small cavities, it is spoken respectively of pulmonary abscess or necrotizing pneumonia.
- Depending on the guest's reaction:
- Purple pneumonia.
- Fibrinose pneumonia.
- Depending on the type of guest:
- Pneumonia in immunocompetent patient.
- Immunodepressed patient pneumonia.
This differentiation can determine a totally different etiological spectrum; The type of immunosuppression, its intensity, and its duration influence the main etiologies to be considered and the differential diagnosis, prognosis, and advisable diagnostic and therapeutic management.
Depending on the scope of acquisition
- Acquired in the community (or extrahospital): It has been defined as an infection of the lungs caused by a wide variety of microorganisms acquired outside the hospital and that determine the inflammation of the lung parenchyma and the alveolar spaces. This type of pneumonia is acquired within the general population and is developed in a non-hospitalized person or in the hospitalized patients who present this acute infection within 24 to 48 hours of their placement.
- Hospital pneumonia or nosocomial (the term is currently preferred pneumonia associated with health care)[chuckles]required] They present greater mortality than community-based pneumonia. At 48 hours or more after hospital admission, diseases that were in the incubation period should be excluded. In the hospital there is the conjunction of a population with alteration of the defense mechanisms, together with the existence of germs very resistant to antibiotics, which creates difficulties in the treatment of the infection.
- NACS (Neumonia associated with health care): It occurs in patients who have been in recent contact with health care, but who are not (or have been in hospital for less than 48 hours)
Prognostic classification
There are two prognostic classifications of pneumonia:
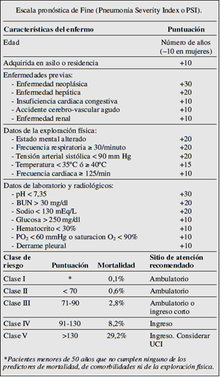
- Fine or PSI classification (pneumonia severity index or PSI)
This classification assigns a score based on 20 parameters; with this score, it is classified in one of the 5 strata, differentiated by their mortality. The strategy of this classification system is based on the fact that 30-day mortality is different for each group. Patients classified in groups I and II are those with the lowest risk, with a mortality of less than 2%, and most can be treated on an outpatient basis. It should be taken into account that a patient under 50 years of age, without any of the diseases listed in the table, with this normal consciousness and without significant alterations in vital signs, it can be assigned to group I, without the need for analytical determinations. On the contrary, the patients classified in groups IV and V are those with the highest risk, with a mortality that oscillates between 15 and 25% and must be admitted. The conduct to follow in patients classified in group III, considered intermediate risk, with a mortality close to 4%, is not yet well defined, they can remain in the emergency department for a period of observation to decide their admission or outpatient treatment.
- Classification CURB65 or CRB65
The CURB65 model (state of Cconsciousness, Uarea value, expiratory R rate, A pressure b>rterial -Blood-, older than 65 years) or CRB65 assesses 5 aspects and age greater than 65 (hence the acronym CURB65), which allows patients to be stratified into 5 severity categories, with chances of death between 0.7% if you have 0 points, to 40% if you have 4 points or more. It is also useful to assess the need for income.
In any case, the decision must be individualized in each case, based on experience and common sense and, whenever possible, must take into account the possibilities of the patient.
Causes
Pneumonia can be caused by one or several etiologic agents:
- Multiple bacteria, like neumococo (Streptococcus pneumoniae), Mycoplasmas pneumoniae, Chlamydias pneumoniae.
- Different viruses.
- Hongos, like Pneumocystis jiroveciShut up.
- Pneumonias are usually caused by: Streptococcus pneumoniae, Staphylococcus aureus and occasionally negative gram bacilos.
- In infants (children from one month to two years) and preschools (children from two years to five years): the main bacterial pathogen is the Streptococcus pneumoniaealso occasionally caused by Chlamydia trachomatis and for the Mycoplasma pneumoniae.
- In children over five years of age: Streptococcus pneumoniae and Mycloplasma pneumoniae.
- In immunocompromised: gramnegative bacteria, Pneumocystis jiroveci, cytomegalovirus (CMV), fungi, and Micobacterium tuberculosis.
- Sometimes pneumonia can occur by anaerobic bacteria, in the case of people who have risk factors to aspire gastric content to the lungs, there is a significant risk of lung abscess.
- In the nosocomial pneumonias: Pseudomonas aeruginosamushrooms and Staphylococcus aureus.
- In adults: Streptococcus pneumoniae and virus influenza.
- In cases of atypical pneumonia: virus, Mycoplasma pneumoniae and Chlamydia pneumoniae.
Various infectious agents—viruses, bacteria, and fungi—cause pneumonia, the most common being:
- Streptococcus pneumoniae: the most common cause of bacterial pneumonia in children.
- Haemophilus influenzae type b (Hib): the second most common cause of bacterial pneumonia.
- Respiratory sincitial virus is the most common cause of viral pneumonia.
- Pneumocystis jiroveci is an important cause of pneumonia in children under six months of HIV/AIDS, responsible for at least one in four deaths of HIV-positive infants.
Signs and symptoms
The following symptoms may be related to the disease:
- Generally, it is preceded by a disease such as flu or common flu.
- Protracted fever for more than three days, particularly if it is high.
- Increased respiratory rate:
- newborns for less than three months: more than 60 per minute,
- infants: more than 50 per minute,
- preschool and school: more than 40 per minute,
- adults: more than 20 per minute.
- There is a sinking or retraction of the ribs with breathing, which can be easily observed with the discovered chest.
- Nasal pits open and close as a quick flush with breathing. (This is mainly given in children).
- Burning in the chest as asthmatic when breathing.
- People affected by pneumonia often have cough that can produce a mucopurulent-type expectoration (yellow), high fever that can be accompanied by chills. Respiratory limitation is also common as well as chest pain of pleuritic characteristics (increases with deep breath and cough). They may also have hemoptisis (blood spread by mouth during cough episodes) and dyspnea. It is often accompanied by commitment from the general state (anorexia, astenia and adinamia).
- The general physical exam is likely to find tachycardia, tachypnea and low blood pressure, whether systolic or diastolic.
- Segmentary physical exam, lung condensation syndrome is often clear:
- a palpation: decrease of expansion and chest elasticity and increase of vocal vibrations;
- to percussion: nuance;
- auscultation: decrease of the vesicular murmur. There can be a picture composed of a tubular murmur surrounded by a crown of crepitating mats.
- The infant patient has cold skin, coughing intensely, seems decayed, can barely cry and may have seizures, gets bitten when coughing, does not want to eat (aphagia), barely reacts to stimuli. The clinical picture is similar in the adult patient.
- In adults over 65 years is likely a symptomatic manifestation much more subtle than found in young people.
Diagnosis
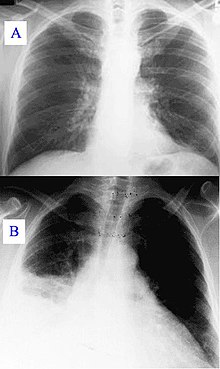
The diagnosis of pneumonia is based both on the patient's symptoms and on the result of the chest x-ray (Rx). Chest X-rays (posteroanterior and lateral), blood tests, and microbiological cultures of sputum and blood are generally used. Chest X-ray is the standard diagnosis in hospitals and clinics with access to X-rays.
In people with other diseases (such as AIDS or emphysema) who develop pneumonia, a chest X-ray can be difficult to interpret. A CT or other tests are often necessary in these patients to make a differential diagnosis of pneumonia.
Forecast
With treatment, most types of bacterial pneumonia will stabilize in 3 to 6 days. Often it takes a few weeks for most symptoms to resolve. Radiographic findings usually disappear within four weeks, and mortality is low (less than 1%). In the elderly or those with other lung problems, recovery may take more than 12 weeks. In people requiring hospitalization, mortality can be as high as 10% and in those requiring intensive care it can be as high as 30-50%. Pneumonia is the most common hospital-acquired infection causing death. Before Arrival of antibiotics, mortality was typically 30% in those who were hospitalized. However, for those whose lung condition deteriorates within 72 hours, the problem is usually due to sepsis. If the pneumonia deteriorates after 72 hours, it could be due to a nosocomial infection or aggravation of other underlying comorbidities. Approximately 10% of patients discharged from the hospital are readmitted due to underlying comorbidities, such as cardiac, pulmonary, or neurological disorders, or due to new-onset pneumonia.
Complications can occur particularly in the elderly and those with underlying health problems. This may include, but is not limited to: empyema, lung abscess, bronchiolitis obliterans, acute respiratory distress syndrome, sepsis, and worsening of underlying health conditions.
Pneumonia is included, by the WHO, among the 10 main causes of death in the world (the fourth cause).
Treatment
Most cases of pneumonia can be treated without hospitalization. Oral antibiotics, rest, fluids, and home care are usually sufficient to complete resolution. However, people with pneumonia who are having difficulty breathing, people with other medical problems, and older people may need more advanced treatment. If the symptoms worsen, the pneumonia does not improve with home treatment, or complications develop, the person often needs to be hospitalized.
Antibiotics are used to treat bacterial pneumonia. In contrast, antibiotics are not helpful for viral pneumonia, although they are sometimes used to treat or prevent bacterial infections that can occur in lungs damaged by viral pneumonia. The choice of antibiotic treatment depends on the nature of the pneumonia, the most common microorganisms that cause pneumonia in the local geographic area, and the underlying immune status and health of the individual.
The treatment of pneumonia should be based on knowledge of the causative organism and its sensitivity to known antibiotics. However, a specific cause for pneumonia is identified in only 50% of people, even after extensive evaluation. In the UK, amoxicillin and clarithromycin or doxycycline are the antibiotics of choice for most patients with community-acquired pneumonia; Patients allergic to penicillins are given a macrolide instead of amoxicillin. In the United States, where atypical forms of community-acquired pneumonia are becoming more common, azithromycin, clarithromycin, and fluoroquinolones have displaced amoxicillin as first-line therapy. The duration of treatment has traditionally been seven to ten days, but there is increasing evidence that shorter courses (as short as three days) are sufficient. According to the Cochrane Library "the effects of treatment remain unclear." duration of antibiotic therapy for community-acquired pneumonia in adolescent and adult outpatients.” Also in children (2 to 59 months) there is currently insufficient evidence to support or question the continued use of antibiotics for treatment of non-severe wheezing pneumonia. Antibiotics for hospital-acquired pneumonia may include vancomycin, third- and fourth-generation cephalosporins, carbapenems, fluoroquinolones, and aminoglycosides. These antibiotics are usually administered intravenously. Multiple antibiotics may be administered in combination, in an attempt to treat all possible causative organisms. The choice of antibiotics varies from hospital to hospital, due to regional differences in the most likely microorganisms, and due to differences in the ability of microorganisms to resist various antibiotic treatments.
In a systematic review it was found that although it is associated with adverse effects such as hyperglycemia, treatment with corticosteroids associated with antibiotics in severe CAP reduced morbidity and mortality, with a number needed to treat (NNT) of 18 (CI 95 % 12- 49).
People who have difficulty breathing due to pneumonia may require extra oxygen. Extremely ill individuals may require intensive care treatment, often including intubation and artificial ventilation.
Viral pneumonia caused by influenza A can be treated with amantadine or rimantadine, while viral pneumonia caused by influenza A or B can be treated with oseltamivir or zanamivir. These treatments are beneficial only if started within 48 hours of the onset of symptoms. Many strains of influenza A H5N1, also known as avian influenza or "bird flu," have shown resistance to amantadine and rimantadine. There are no known effective treatments for viral pneumonias caused by SARS coronavirus, adenovirus, hantavirus, or parainfluenza virus.
| Histologic subtype | Frequency (%) | Antibiotic | |
|---|---|---|---|
| Streptococcus pneumoniae | 31.1 | In healthy adults:
Comorbidities:
| |
| Staphylococcus aureus | 0.4 |
| |
| Moraxella catarrhalis | 0.4 |
| |
| Streptococcus pyogenes | 0.4 |
| |
| Neisseria meningitidis | 0.4 |
| |
| Klebsiella pneumoniae | 0.4 |
| |
| Haemophilus influenzae | 0.4 |
| |
| Atypical pneumonia | Legionella pneumophila | 23.2 | |
| Mycoplasma pneumoniae | 3.0 | ||
| Chlamydophila pneumoniae | 1.2 | ||
| Pneumocystis jiroveci | 10.7 | ||
| Tuberculosis | 0.4 | ||
Contenido relacionado
Complement system
Santiago Ramon y Cajal
Friedreich's ataxia